Table of Contents
- Why It Is Important to Use Clean Needles and Other Injection Equipment
- How to Reduce HIV Risk When Injecting Drugs
- Drug Treatment Programs
- New Needles
- Needle Exchange Programs
- Cleaning Injection Equipment
- Taking Care of Yourself and Others
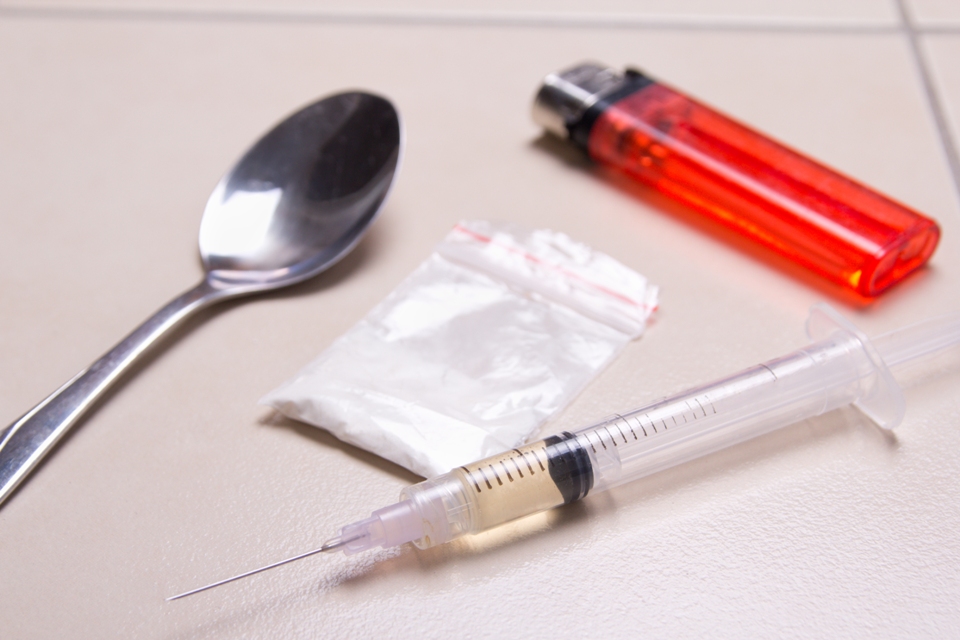
Why It Is Important to Use Clean Needles and Other Injection Equipment
Sharing Needles and HIV Acquisition
Injection drug use (IDU) accounts for a large number of HIV cases worldwide. Sharing needles, syringes, and drug injection equipment or "works" (including cookers and cotton) allows HIV to be spread from one person to another. The World Health Organization (WHO) estimates that about 11 million people inject drugs worldwide, and that 1.4 million of them are living with HIV. Globally, one out of every ten new HIV transmissions is through injection drug use. However, that average is much higher in some areas.
Drug treatment programs are available in many countries to help you stop injection drug use.
Blood from a person living with HIV can remain in or on a needle or syringe and then be transferred directly to the next person who uses that same needle or syringe. Blood that contains HIV can also find its way into drug solutions through:
- Using syringes that have even very small amounts of blood on them to prepare drugs
- Reusing water
- Reusing bottle caps, spoons, or other containers ("cookers") used to dissolve drugs in water and to heat drug solutions
- Reusing small pieces of cotton or cigarette filters ("cottons") to filter out particles that could block the needle
Hepatitis
People who inject drugs also risk getting hepatitis B (HBV) and C (HCV), both of which are diseases that damage the liver and are spread through blood. HCV is common in people who inject drugs – the WHO estimates that four in ten people who inject drugs around the world are living with HCV.
Hepatitis is easily spread through sharing needles and other injection supplies, such as cookers, cotton, and ties. Cleaning your skin before you inject is important. Also make sure to throw away alcohol pads and cotton wipes so that no one else touches them. If possible, wipe down surfaces before injecting. If new needles and injection equipment are not available, cleaning your injection drug equipment with bleach according to the directions below can kill HBV; it is unclear whether it can kill HCV.
The best way to prevent hepatitis is to use a new needle and syringe each time, and never share any part of your works. It is important to get routinely tested for hepatitis A, B, and C. Ask your healthcare provider about your risks for getting these types of hepatitis. If available, get vaccinated against hepatitis A and B to prevent infection with these two types of the virus; there is no vaccine to prevent hepatitis C.
Bacterial Infections
Injecting drugs and other substances can cause other bacterial infections, especially skin infections. Bacteria can also enter the body, affecting bones and joints, as well as the heart (a condition called endocarditis). When the bacteria reach the heart or its surrounding tissue, they can cause life-threatening events, such as heart failure or stroke. To help prevent such infections, make sure you clean the skin where you intend to inject, use new sterile needles and syringes, if possible, or clean used needles and equipment as described below, if sterile syringes and needles are not available.
How to Reduce HIV Risk When Injecting Drugs
If you inject drugs, you can reduce your risk of getting HIV and/or hepatitis by:
- Using drug treatment programs to get help with quitting
- Using a new, sterile needle and syringe every time and not sharing needles, syringes, cookers, or cotton with others
- Using needle exchange programs to get new unused needles and syringes, etc.
- If new, unused needles and syringes are not available, thoroughly cleaning used ones before another person uses them (for instructions, see below). The Additional Resources section at the end of this fact sheet also has videos about how to clean syringes.
Drug Treatment Programs
Stopping injection drug use altogether is probably the best thing you can do for your health. This may be an incredibly hard thing to do, and it may not work for everyone. However, it will remove all risk of acquiring HIV and hepatitis from sharing needles, syringes, cookers, and cottons.
Drug treatment programs are available in many countries to help you stop injection drug use. Some programs have waiting lists and people with children may need to make special arrangements. To find out if this a good option for you, look for a substance use treatment program in your area. See the Additional Resources section below for help in finding a program. Also see our fact sheet on Substance Abuse and Addiction for more information on the link between substance use and HIV and what you can do if you are struggling with substance abuse.
New Needles
If you do inject drugs, it is best to use a new, sterile needle and syringe every time you inject and not share needles and syringes with others. You might not think of yourself as having "shared" a needle and syringe if both you and a close friend or acquaintance used them. But sharing needles and syringes with friends can be as dangerous as sharing with strangers.
The WHO strongly supports the use of evidence-based needle and syringe programs as part of HIV prevention.
"Street sellers" of needles and syringes may repackage used needles and syringes and sell them as sterile when they are not. Do not assume a needle and syringe are new, even if they seem to be packaged as new.
Get needles and syringes from reliable sources, such as pharmacies. In many parts of the US you can purchase sterile needles and syringes without a prescription from a local pharmacy.
Needle Exchange Programs
If you cannot buy new needles and syringes from a pharmacy, look for a needle exchange program (also called a syringe exchange program or syringe service program). Needle exchange programs can give new syringes and needles to people who inject drugs to prevent the spread of HIV and other diseases that are transmitted through blood.
Although scientific evidence shows needle exchange programs reduce the spread of HIV and do not increase drug use, some people are against them. The WHO strongly supports the use of evidence-based needle and syringe programs as part of HIV prevention. There are needle exchange programs in some countries, but they are not available everywhere. In the US, some states have needle exchange or syringe access programs, while others do not.
If you have to share, thoroughly clean your needles and works with bleach and water after each use and before reusing.
Needle exchange programs offer a good way for people who inject drugs to reduce the risk of HIV transmission. In addition, these programs may be able to help you get benefits, medical care, and access to drug treatment programs. You can search for a needle exchange program in the US by clicking here.
Cleaning Injection Equipment
If you must share needles and syringes because new, unused ones are not available, always clean the needles and syringes with bleach and water immediately after use and just before using them again. Keep in mind that cleaning with bleach does not make re-using the equipment risk-free. However, it is an important tool to reduce the risk of infection. To be effective, you must carefully follow the cleaning procedures listed below every time.
Part One
Pour clean water into a cup, cap or something that only you will use.
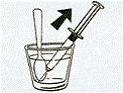
Fill the syringe by drawing the water up through the needle to the top of the syringe.
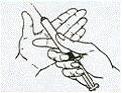
Shake it around and tap it to loosen the blood.
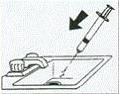
Squirt out the water and repeat at least three times (do not reuse water).
Part Two
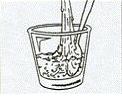
Pour some undiluted (full-strength, no water added) bleach into a cup, cap or something that only you will use.

Fill the syringe by drawing the bleach up through the needle to the top of the syringe.

Shake it around and tap it. Leave the bleach in the syringe for at least 30 seconds.

Squirt out the bleach and repeat at least three times (do not reuse bleach).
Part Three

Pour new clean water into a cup, cap or something that only you will use. Don't use the water from part one.

Fill the syringe with water, to rinse out the bleach. Fill the syringe by drawing the water up through the needle to the top of the syringe.

Shake it around and tap it for at least 30 seconds.

Squirt out the water and repeat three times (do not reuse water).
Some tips:
- You can make the cleaning work better by taking the syringe apart, removing the plunger from the barrel and soaking the parts in bleach for at least 30 seconds.
- Never shoot or drink the bleach
- If the cooker (spoon) must be reused, soak it in bleach for at least 30 seconds and then rinse it with clean water
- Since bleach gets weaker when it is exposed to light, store all bleach for cleaning needles and works in a container that does not let light pass through
Taking Care of Yourself and Others
Sharing a needle, syringe, or any related equipment for any use, including skin popping, tattooing, body piercing, or injecting steroids or hormones, can put you at risk for acquiring HIV or other blood-borne infections. If you plan to have a body piercing or get a tattoo, make sure you go to a qualified technician who uses sterile equipment.
The safest thing to do is to stop injecting drugs altogether. If this is not possible right now, get new, sterile needles each time you shoot up or find a needle exchange program. If you have to share, thoroughly clean your needles and works with bleach and water after each use and before reusing.
If you are at risk because you are injecting drugs now or have injected in the past, get tested for HIV and hepatitis. You can also put your sexual partners at risk if you have unprotected sex, so it is important to use condoms and practice safer sex.
The original version of this article (2006) was adapted from materials from the San Francisco AIDS Foundation and the University of Albany.
Illustrations from Heart of Richmond AIDS Society (https://www.facebook.com/HeartOfRichmondAidsSociety/)

