Table of Contents
- What Are Microbicides?
- How Would Microbicides Work?
- Are Microbicides Currently Available?
- What is Happening in Microbicide Research?
- Would Microbicides Eliminate the Need for Condoms?
- Would Microbicides Protect Against All Sexually Transmitted Infections?
- What if a Woman Wants to Get Pregnant?
- Would Microbicides Be Safe?
- How Would Microbicides Benefit Men?
- How Would Microbicides Benefit Women Living with HIV?
- Why Do We Need Microbicides if We Will Eventually Have an HIV Vaccine?
- How Much Will Microbicides Cost, and Will People Be Able to Afford Them?
- What About Nonoxynol-9 (N-9)?
- Taking Care of Yourself
What Are Microbicides?
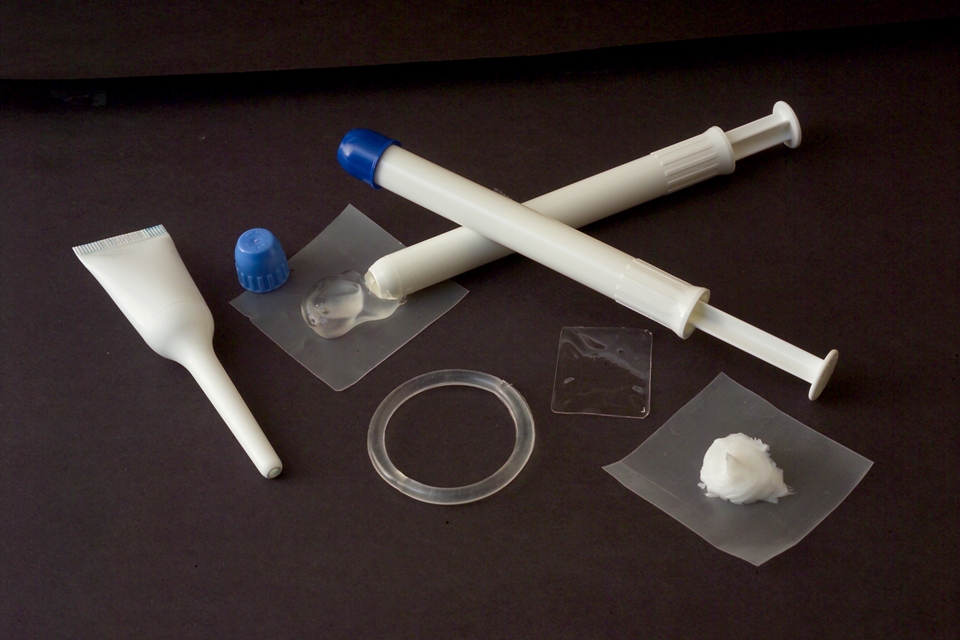
Microbicides are products for reducing the transmission of HIV and/or other sexually transmitted infections or diseases (STIs or STDs). They are still being developed. Microbicides could come in many forms, including gels, creams, suppositories, films, lubricants, sponges, or vaginal rings. They could be used in the vagina or rectum ("butt").
One microbicide for HIV prevention, dapivirine, is currently available in some countries in Africa as a vaginal ring, but it has not been approved in the US.
How Would Microbicides Work?
Microbicides could work in different ways:
- Killing germs, such as bacteria and viruses, or making them inactive
- Changing the condition of the vagina or rectum to make infection less likely
- Blocking infection by creating a barrier between the germ and the cells of the vagina or rectum
- Preventing the germ from spreading after it has entered the body
Are Microbicides Currently Available?
The World Health Organization recommends a vaginal ring containing the microbicide dapivirine for HIV prevention in people with vaginas. It has been approved in some sub-Saharan countries, and the European Medicines Agency has issued a favorable opinion. However, the ring has not been approved in the US. See also Vaginal Rings below.
What is Happening in Microbicide Research?
Microbicides have been in development for more than 20 years. Early studies did not find an effective microbicide. However, there is hope that new microbicides that contain HIV drugs will be more effective. These microbicides come in several different forms – gels, rings, films – and may serve as multipurpose prevention technologies (MPTs), which address two or more sexual health issues at one time (e.g., HIV and pregnancy).
Researchers are studying several methods for combining prevention technologies, including a vaginal ring that contains both a hormonal contraceptive (to prevent pregnancy) and an HIV drug (to prevent HIV).
Vaginal Rings
There is also hope that vaginal rings containing HIV drugs can prevent HIV transmission. The ring is flexible and can be inserted by the woman herself deep inside the vagina against the cervix (entrance to the womb). The ring is comfortable and rarely felt by the woman herself or her sexual partner(s). It needs to be replaced every one to two months. This is different from vaginal gels, which need to be inserted directly before or at the time of sex. Women are in control when they use either rings or gels. However, with the ring, women do not need to plan for sex.
In January 2021, the World Health Organization recommended the dapivirine ring for women at substantial risk of acquiring HIV.
Two studies of a vaginal ring that contains dapivirine – an HIV drug called a non-nucleoside reverse transcriptase inhibitor (NNRTI) – showed a modest reduction in women acquiring HIV, but little benefit to younger women. Many younger study participants did not use the ring as prescribed – were not adherent – and therefore saw little protection. However, adherence increased over time, suggesting that women may have needed some time to become familiar with the new technology.
In January 2021, the World Health Organization recommended the dapivirine ring for women at substantial risk of acquiring HIV. The ring has been approved in some countries in Southern Africa, and applications for approval are pending elsewhere. However, the US Food and Drug Administration is no longer considering the ring for approval.
Vaginal and Rectal Gels
Studies of a gel that contains the HIV drug Viread (tenofovir) and is inserted into the vagina have shown conflicting results. While the gel seemed promising at first, a second study was stopped early because it did not prevent acquisition of HIV. However, this was mostly because women did not use the gel as they had been told to do. Researchers are now trying to understand why so few women used this gel as directed to help them identify more acceptable and effective prevention methods.
A version of the tenofovir gel designed for rectal (in the "butt") use has also been tested. Overall, more participants who were told to use the gel only before and after sex used it properly compared to participants who were told to use it every day. Rectal gels containing dapivirine and maraviroc (two HIV drugs) are currently in development or being tested. Scientists are also studying vaginal gels containing dapivirine, dapivirine plus maraviroc, and dapivirine plus darunavir.
Vaginal Films
A vaginal film with dapivirine delivered enough drug to vaginal tissue to prevent HIV acquisition when it was tested in the laboratory. Research into this film continues.
Multipurpose Prevention Technologies (MPT)
MPTs provide ways of preventing more than one thing in a single device. For example, MPTs may prevent pregnancy and HIV, or they may prevent HIV and several other STIs. Having methods that combine prevention of pregnancy and sexually transmitted infections (including HIV) would be more convenient, and likely lead to more consistent, and therefore more effective, use.
Researchers are studying several methods for combining prevention technologies, including a vaginal ring that contains both a hormonal contraceptive (to prevent pregnancy) and an HIV drug (to prevent HIV; a form of Pre-Exposure Prophylaxis, or PrEP). It can be inserted well before sex, stay in the vagina for up to three months, and is not usually felt by either partner. Vaginal gels that may prevent pregnancy and HIV, as well as one that may prevent HIV and two other STIs are also under investigation.
Would Microbicides Eliminate the Need for Condoms?
Microbicides could be used without the knowledge of women's sexual partners, which would put the power of prevention directly in women's hands.
No. When used consistently and correctly, male or female condoms are likely to provide better protection against HIV and other STIs than microbicides, so they are still the best choice. Even with recent research showing that people living with HIV who are taking HIV medications and whose viral load is too low to be measured with standard tests do not transmit the virus to their sexual partners, condoms are still the best protection against all STIs.
But for people who do not have access to condoms, or who cannot or will not use condoms, microbicides would provide another option. This is especially true for women whose male partners refuse to use condoms. Microbicides could be used without the knowledge of women's sexual partners, which would put the power of prevention directly in women's hands. Using microbicides could save lives and help reduce HIV transmission.
Would Microbicides Protect Against All Sexually Transmitted Infections?
Many of the microbicides being tested work against HIV. In time, a product may be developed that combines different microbicides and could prevent a wide range of STIs, including HIV (see multipurpose prevention technologies, or MPTs, above).
What if a Woman Wants to Get Pregnant?
Many of the microbicides being studied would allow a woman to get pregnant. These are called non-contraceptive microbicides. They would offer women the option of getting pregnant while still protecting themselves from acquiring HIV – an option that is not available with condom use. The tenofovir gel mentioned above is one example of a non-contraceptive microbicide. Contraceptive microbicides or MPTs would prevent pregnancy as well as HIV and, ideally, other STIs. It is important to have both types available.
Would Microbicides Be Safe?
Any new product must go through strict safety testing before becoming available to the public. Health activists and researchers are closely watching the clinical testing of microbicides to make sure that they are tested correctly.
How Would Microbicides Benefit Men?
It is possible that the male partner of a woman living with HIV could be protected from acquiring HIV if she used a vaginal or rectal microbicide. However, this would need to be tested in clinical trials. Vaginal microbicides must be tested separately from rectal microbicides.
How Would Microbicides Benefit Women Living with HIV?
Microbicides could help protect women living with HIV from acquiring other HIV strains, from other STIs, and from pregnancy.
Why Do We Need Microbicides if We Will Eventually Have a Vaccine to Prevent HIV?
Research on developing a vaccine to prevent acquisition of HIV has not been successful so far. One microbicide is already available in some countries, and others may follow sooner than a vaccine. Even if a safe and effective vaccine is discovered, vaccines and microbicides will both have roles to play in the prevention of HIV.
How Much Will Microbicides Cost, and Will People Be Able to Afford Them?
Advocates are working with researchers and policy makers to make sure that any approved microbicide will be as affordable and accessible as possible.
What About Nonoxynol-9 (N-9)?
N-9 products are sold over the counter as spermicides that can prevent pregnancy. They cannot prevent the transmission of HIV or other sexually transmitted infections. In fact, when used more than once a day, N-9 contraceptive products may actually increase the risk of acquiring HIV by irritating the lining of the vagina. Other studies show that N-9 is even more irritating to the rectum than to the vagina.
According to the World Health Organization (WHO):
- N-9 is not effective at preventing the transmission of HIV or other STIs. It should NOT be used for that purpose.
- Women at risk for acquiring HIV, especially those having sex more than once a day, should NOT use N-9 for birth control.
- Condoms with N-9 provide no more protection against pregnancy or infection than plain lubricated condoms. Since N-9 condoms may cause irritation, they should not be used.
- Products with N-9 should NEVER be used for anal sex.
Taking Care of Yourself
Until microbicides are widely available, the best way to protect yourself or your partner from acquiring HIV is for the partner living with HIV to be on effective HIV treatment. If their viral load stays undetectable, they cannot transmit HIV to a sexual partner. For the HIV-negative partner, PrEP is also an option. Using a male or female condom prevents other STIs, including HIV, and is another option. Reducing your number of partners will also reduce your risk of acquiring HIV. It is also important to avoid the use of nonoxynol-9 products if you think there is any chance you may be exposed to HIV. Getting tested for STIs regularly and getting treatment quickly if you have an STI will also help reduce your risk of acquiring HIV if you are exposed to the virus.

